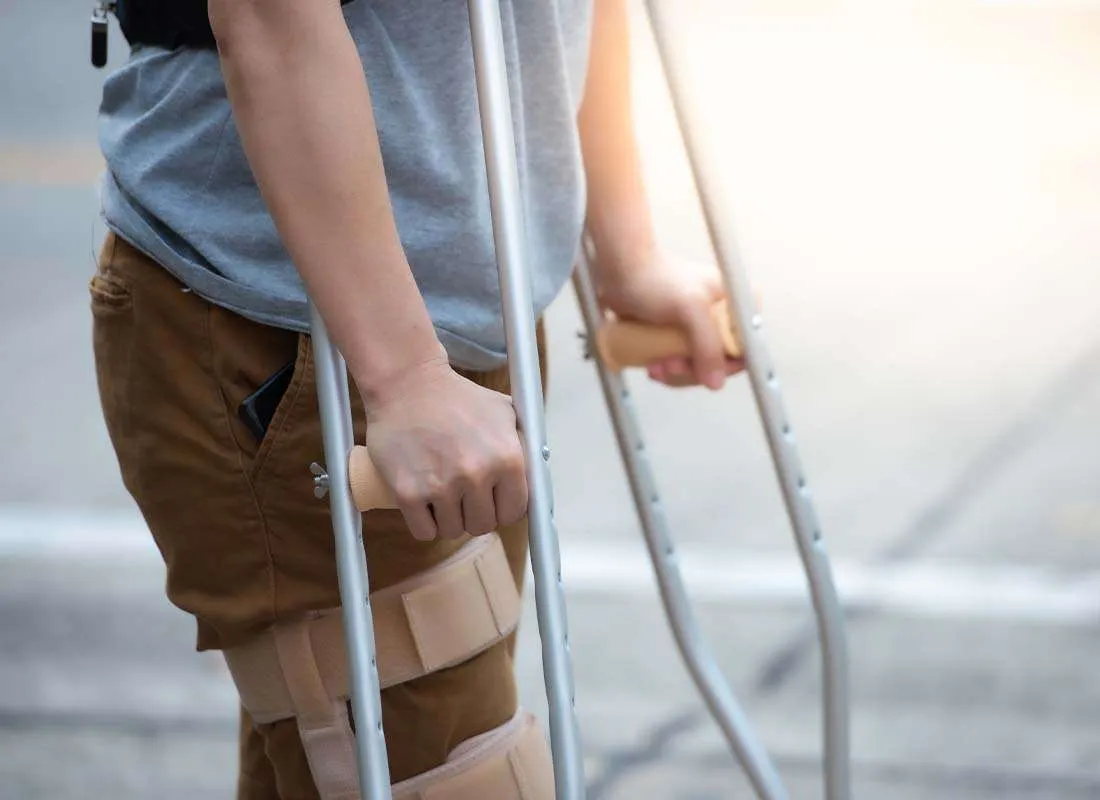
When someone faces a health condition that prevents them from working, the difference between short term and long term disability benefits suddenly becomes very important. Many people only start asking questions after a disability claim denied decision leaves them searching for answers. While both types of coverage are designed to replace lost income, they operate differently in terms of timing, eligibility, and long term expectations.
Contents
What Short Term Disability Covers
Short term disability benefits are designed to provide income replacement for a limited period, usually following an illness, injury, or medical procedure. Coverage often begins after a brief waiting period, sometimes just a few days or weeks. These benefits typically last anywhere from a few weeks to several months, depending on the policy.
The goal of short term coverage is to support recovery during a temporary absence from work. Because of this, the approval process is often more straightforward. Medical evidence is still required, but insurers generally focus on whether the claimant cannot perform their current job for a short period of time.
How Long Term Disability Differs
Long term disability benefits come into play when a condition extends beyond the short term coverage period. These benefits are designed for more serious or prolonged conditions that prevent a person from returning to work for an extended time. Payments can continue for years, or even until retirement age, depending on the policy.
The review process for long term benefits is typically more detailed. Insurers look closely at medical records, functional limitations, and the likelihood of recovery. Over time, the definition of disability may change from being unable to perform one’s own job to being unable to perform any suitable work. This shift makes long term claims more complex.
Waiting Periods and Transitions
One key difference between the two types of benefits is how they connect. Short term disability often acts as a bridge until long term coverage begins. Once short term benefits end, there is usually a waiting period before long term benefits start. During this transition, claimants must provide updated medical evidence to show that their condition continues to prevent them from working.
This transition stage can be challenging. A claim that was approved in the short term does not guarantee approval for long term benefits. Insurers may take a closer look at the file and apply stricter criteria before continuing payments.
Differences in Evidence Requirements
Short term claims often rely on initial medical assessments and basic documentation. In contrast, long term claims require more comprehensive evidence. Detailed reports from specialists, ongoing treatment records, and clear descriptions of functional limitations become increasingly important.
Insurers may also request independent assessments or additional evaluations for long term claims. The expectation is that the evidence will clearly support the severity and duration of the condition over time.
Why the Distinction Matters
Understanding the differences between short term and long term disability benefits helps set realistic expectations. It explains why a claim that seems straightforward at first can become more complex later. Being aware of the stricter requirements for long term coverage can also help claimants prepare stronger applications and avoid common pitfalls.
Conclusion
Short term and long term disability benefits serve different purposes, even though they are closely connected. One provides immediate support during temporary absences, while the other addresses more lasting conditions that prevent a return to work. Recognizing how these systems operate can help individuals better prepare for each stage and improve their chances of maintaining consistent financial support.